By
Liz Highleyman
Since
the advent of effective combination
ART in the mid-1990s, several studies have observed
an elevated rate of heart attacks and other cardiovascular
events in people with HIV. Some studies have linked heart
risk to specific antiretroviral drugs or drug classes --
including protease inhibitors and the nucleoside reverse
transcriptase abacavir
(Ziagen, also in the Epzicom
and Trizivir
coformulations) -- but data are not consistent, and some
have found an elevated risk in HIV positive people who are
not on treatment.
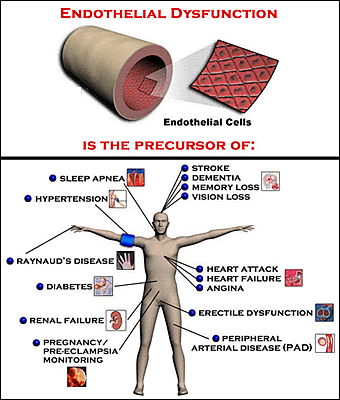
In
the present study, Danish researchers investigated whether
peripheral endothelial vasomotor function (ability of blood
vessels to dilate and contract) changed when treatment-naive
HIV patients started ART.
This
prospective longitudinal analysis included 9 previously
untreated participants. All were men and the median age
was 51 years. Median duration of HIV infection was about
2 years and the mean baseline CD4 count was 260 cells/mm3.
After 6 months on their first ART regimen, all achieved
complete viral suppression and the mean CD4 count increased
to 402 cells/mm3.
Most
of the participants (7 of 9) started a regimen of efavirenz
plus tenofovir/emtricitabine (the drugs in the Atripla coformulation),
with 1 starting abacavir/lamivudine
(the drugs in the Epzicom coformulation) and 1 starting
zidovudine/lamivudine
(the drugs in the Combivir coformulation).
Vasomotor
function was assessed by measuring flow-mediated dilation
(FMD) and nitroglycerin-mediated dilation (NMD) of the brachial
artery in the upper arm using high-resolution Doppler ultrasound.
FMD refers to how well blood vessels respond to changes
in blood flow; nitroglycerin is a drug used to expand blood
vessels. Study participants were examined before and 1 month
after ART initiation. Brachial artery scans were recorded
at rest and during increased blood flow caused by inflating
and deflating a cuff (as done when measuring blood pressure,
but for a longer period of 4.5 minutes).
Results
 |
1
month after ART initiation, flow-mediated dilation decreased
significantly, from 8.7% to 4.6% (P = 0.027). |
 |
FMD
remained impaired at the end of the 6 month follow-up
period (5.1%; P = 0.064). |
 |
Nitroglycerin-mediated
dilation increased slightly, but the change did not
reach statistical significance (12.8% vs 14.3% at 1
month; P = 0.21). |
 |
Blood
lipid levels were not significantly different at 6 months
compared with baseline. |
These
findings led the investigators to conclude that, "FMD
decreases 1 month after initiation of ART in treatment-naive
HIV patients."
"This
indicates that ART initiation leads to endothelial dysfunction,
which could be a mechanism involved in the increased risk
of cardiovascular disease found in recent observational
studies," they continued.
Another
recent study indicated that patients taking abacavir
had a greater decrease in FMD, but HIV patients on ART overall
had below normal levels. Further study is needed to determine
the mechanism by which antiretroviral drugs might cause
endothelial dysfunction, as well as the role of chronic
inflammation due to HIV infection itself.
Copenhagen
University Hospital, Rigshospitalet, Copenhagen, Denmark;
University of Copenhagen, Copenhagen, Denmark; Hvidovre
University Hospital, Denmark; Frederiksberg University Hospital,
Denmark.
10/20/09
References
US
Kristoffersen, A-M Lebech, N Wiinberg, and others. Peripheral
Endothelial Function is Reduced after Initiation of Antiretroviral
Therapy in Treatment Naïve HIV Patients: A Prospective
Longitudinal Study. 49th Interscience Conference on Antimicrobial
Agents and Chemotherapy (ICAAC 2009). San Francisco. September
12-15, 2009. Abstract H-1579.